Can I Get My Teeth Whitened If They Are Sensitive?
Dreaming of white teeth but nervous about making your sensitive teeth even harder to deal with? Or maybe your sensitive toothpaste that promises a brighter smile is just not cutting it. Tooth sensitivity is one of the most common reasons people put off professional whitening, and once you find what works, it can be intimidating to introduce anything into your routine, even dentist-recommended products.
What many sensitivity sufferers don’t realise is that professional teeth whitening for sensitive teeth is possible. Sensitivity is rarely a dealbreaker; instead, it’s a factor to manage, and with the right approach, most people can still achieve a noticeably whiter smile.
This article covers why whitening causes sensitivity, why professional treatment is a different proposition from anything you’ll find over the counter, and what to expect from the whitening options at KB Village Dental if sensitivity is a concern for you.
So, Can You Whiten Sensitive Teeth?
In most cases, yes. But what matters is understanding why your teeth are sensitive before treatment begins, because the cause shapes everything: the product, the concentration, the session length.
Not everyone is a suitable candidate right away. Active tooth decay, cracked teeth, inflamed gums, or severe gum exposure or recession need to be treated first. Whitening over an untreated problem won’t just produce poor results; it can make things worse. A proper assessment before treatment isn’t optional; it’s what makes a safe outcome possible.
Why Does Teeth Whitening Cause Sensitivity?
Whitening gels use hydrogen peroxide or carbamide peroxide to penetrate the enamel and break down stain molecules within the tooth. During this process, the peroxide can temporarily reach the dentinal tubules, microscopic channels that connect the outer tooth surface to the nerve. When these tubules are stimulated, you get that familiar zingy or achy feeling.
For people with healthy enamel, the effect is mild and short-lived, usually resolving within 24 to 48 hours. For people who already experience sensitivity due to enamel wear, gum recession, or exposed dentin, there’s less of a protective buffer, meaning it can feel more pronounced.
It helps to separate two different things here. Pre-existing sensitivity means your teeth are already reactive before whitening begins. Mild cold sensitivity from minor enamel wear is a very different situation from significant dentinal hypersensitivity from gum recession or exposed roots. The former might only require a modified product or shorter sessions; the latter warrants a closer look before any whitening proceeds.
Whitening-induced sensitivity is the temporary discomfort that’s a normal part of the process. Expected, manageable, and not a sign that anything has gone wrong.
Why Professional Whitening Matters More When You’re Sensitive
Over-the-counter teeth whitening toothpastes, whitening strips and kits are widely available in Australia, but if you have sensitive teeth and have tried one only to end up in discomfort, that experience isn’t representative of what professional whitening treatments feel like.
It’s also worth addressing a common misconception. Products marketed as “gentle” or “natural” — activated charcoal toothpastes and non-peroxide whitening systems in particular — are often more abrasive than correctly managed peroxide teeth whitening treatment. For sensitive teeth, abrasive products can accelerate enamel wear and worsen underlying sensitivity over time. Gentle-sounding doesn’t always mean gentle in practice.
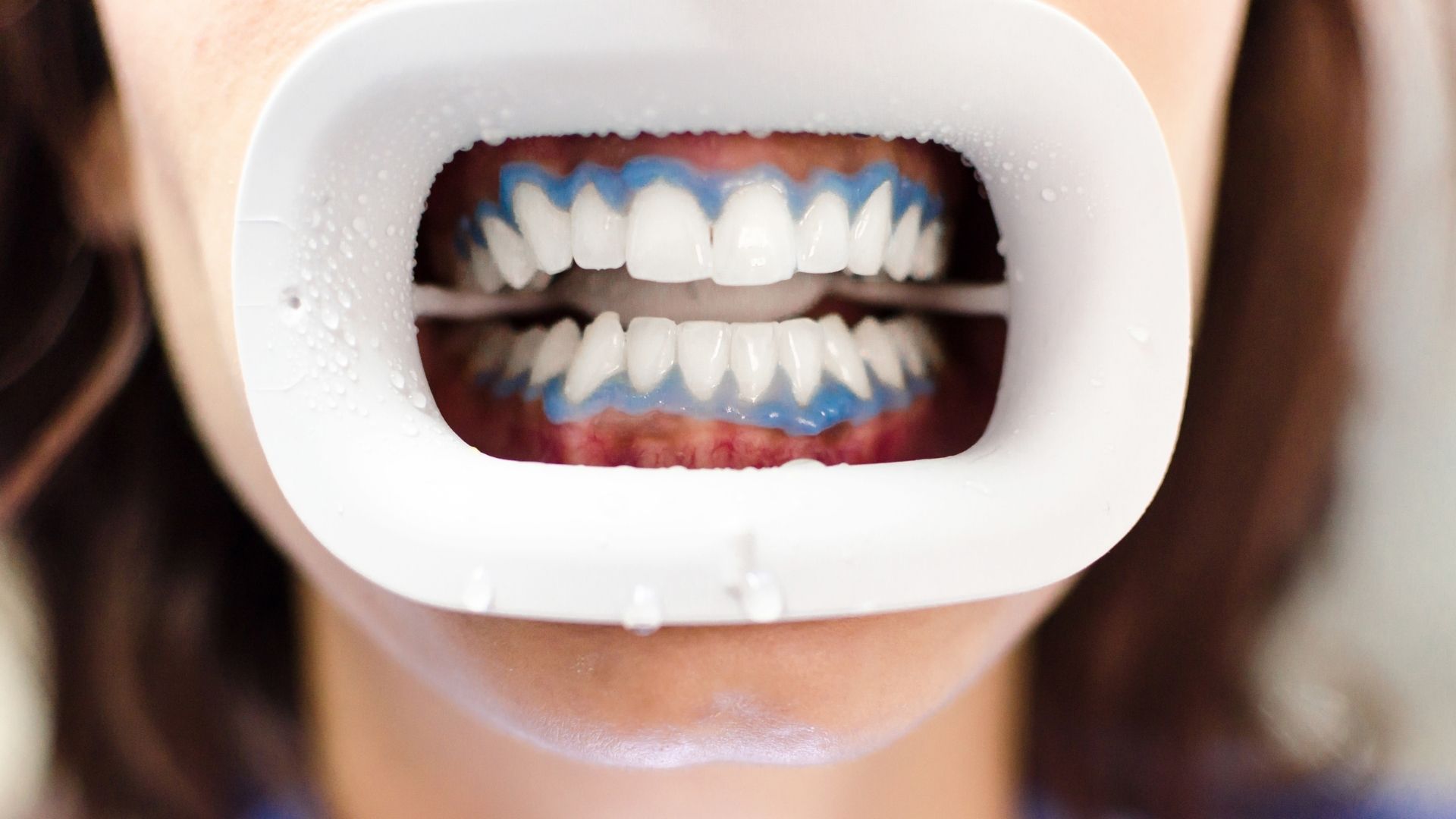
Professional whitening is different for a few reasons. In Australia, the TGA caps home-use hydrogen peroxide at 6% for OTC products. Dental clinics can use significantly higher concentrations because the process is fully supervised. Your oral health is assessed first. Desensitising agents like potassium nitrate and fluoride are applied before and after treatment. Custom trays keep the gel on your teeth rather than spilling onto gum tissue, and if you’re uncomfortable at any point, treatment stops.
Whitening for Sensitive Teeth at KB Village Dental
At KB Village Dental, Dr Evan uses two professional systems: Philips Zoom! WhiteSpeed for in-chair treatment and Opalescence for take-home whitening with custom trays.
Philips Zoom! WhiteSpeed can lighten teeth by up to eight shades in a single 45-minute session. The Zoom! formula includes Amorphous Calcium Phosphate (ACP), a remineralising compound built into the system specifically to reduce sensitivity during and after treatment. For patients who’ve had uncomfortable experiences with other whitening products in the past, this is a meaningful difference; it’s not sensitivity management bolted on afterwards, it’s part of how the system is designed.
Opalescence take-home whitening uses custom-fitted trays made from impressions of your teeth, paired with professional-grade gel. Opalescence contains both potassium nitrate and fluoride, built-in desensitisers that protect enamel and calm nerve response throughout the process. Many sensitive-teeth patients prefer whitening in the comfort of their own home, and Opalescene allows exactly that, with lower concentrations applied gradually over one to two weeks.
Which suits you best depends on your sensitivity level, oral health, and how quickly you’d like results. When you come in, Dr Evan will review your oral health, review your sensitivity history, and check any existing restorations before making recommendations. The point of that conversation is to ensure you understand your options and feel confident in your decision, not to push you toward a particular treatment.
Patients with existing restorations should also know that whitening gel works only on natural enamel. Fillings, crowns, and veneers won’t lighten. If you have tooth-coloured restorations in your smile zone, it’s worth discussing at your consultation, so expectations are well-matched from the start.
Reducing Sensitivity Before and After Teeth Whitening
A few practical steps can make a real difference to your experience.
Before treatment, use a potassium nitrate-based sensitivity toothpaste — like Sensodyne — for at least 2 weeks. This helps block dentinal tubules and reduces baseline nerve reactivity before whitening begins. Flag any existing dental concerns to Dr Evan at your consultation.
During take-home treatment, wear your trays for shorter sessions initially and build up gradually. And unless specifically instructed, don’t sleep in your trays. Prolonged contact with the gel increases the risk of sensitivity and gum irritation.
After treatment, avoid very hot or very cold foods or drinks, as well as acidic foods and drinks, for 24 to 48 hours. Keep using your sensitive toothpaste for at least a week after treatment, and use any fluoride gel as directed. Some sensitivity in the day or two after whitening is normal. But if it persists beyond a week, book a follow-up.
When Whitening Isn’t the Right First Step
Sometimes the honest answer is: not yet. If an assessment finds active decay, a cracked tooth, exposed roots, or significant gum disease, whitening should wait until those issues are resolved.
In some cases, unexplained or severe sensitivity is itself a symptom of an underlying problem, and whitening in those circumstances could cause real harm. Where whitening isn’t appropriate, or where discolouration stems from internal causes that don’t respond to peroxide (such as certain medications, trauma, or tetracycline staining), Dr Evan can talk through alternatives like dental veneers or crowns, depending on what’s driving the concern.
Talk to the Team at KB Village Dental
KB Village Dental is at 19 Broughton Street, Kirribilli, and is easy to get to for patients from Milsons Point, Neutral Bay, Crows Nest, Mosman, and McMahons Point. To find out whether professional whitening is right for you, or discuss what it will take to achieve a brighter smile, book a consultation online or call (02) 9964 9166.
Any dental procedure carries potential risks and benefits. Before proceeding with teeth whitening, please consult with a qualified dental professional to determine the most appropriate treatment for your individual circumstances.
Frequently Asked Questions
Is teeth whitening safe for sensitive teeth?
Yes, for most people. The key is having a proper assessment before treatment begins, so the cause of your sensitivity is understood. Sensitivity alone doesn’t disqualify you from whitening, but it does mean the approach needs to be tailored to your situation. Untreated decay, teeth grinding, cracked teeth, or active gum disease should be addressed first so your dentist can safely whiten teeth and minimise discomfort. Under professional supervision, with the right product and concentration, whitening can be safe and effective even for patients who experience regular sensitivity.
What teeth whitening method is recommended for sensitive patients?
It depends on the severity of your sensitivity. At-home whitening with custom trays, such as Opalescence, is often well-suited to sensitive patients because it uses lower peroxide concentrations applied gradually over one to two weeks, which tends to produce less discomfort than a single high-concentration in-chair session. That said, in-chair systems like Philips Zoom! WhiteSpeed includes Amorphous Calcium Phosphate (ACP) technology designed to reduce sensitivity during treatment, making it a viable option for many sensitive patients, too. Dr Evan will assess your sensitivity history and oral health before recommending the best approach for you.
How much does teeth whitening cost in Australia?
Professional teeth whitening costs vary depending on the method and the clinic. In-chair whitening generally sits at a higher price point than take-home kits due to the chair time, professional supervision, and strength of the systems used. Over-the-counter products are cheaper upfront, but for patients with sensitive teeth, they carry a higher risk of discomfort and less predictable results. For specific pricing on Philips Zoom! and Opalescence treatments at KB Village Dental, call the clinic on (02) 9964 9166 or book a consultation online.
What whitening agents are recommended for those who experience tooth sensitivity?
Professional whitening gels that include built-in desensitisers are the best starting point. Opalescence gel contains both potassium nitrate and fluoride, which help calm nerve response and protect enamel during the whitening process. Potassium nitrate works by blocking dentinal tubules (the channels that allow whitening agents to reach the tooth nerve), reducing the zingy sensation many people experience. For in-chair treatment, the ACP formula in Philips Zoom! serves a similar remineralising purpose. Using a potassium nitrate-based desensitising toothpaste, such as Sensodyne, along with a soft-bristled toothbrush, for 2 weeks before treatment can also reduce baseline sensitivity.
Can teeth whitening worsen sensitivity?
It can, if done incorrectly or too frequently. Using high-concentration products without professional guidance, over-whitening, or abrasive “natural” alternatives like charcoal toothpaste can all damage enamel and worsen underlying sensitivity over time. Some temporary sensitivity after a whitening session is normal and usually resolves within 24 to 48 hours. But if sensitivity increases noticeably after repeated treatments, or persists beyond a week, that’s worth discussing with your dentist. Professional treatment reduces this risk significantly because concentration, frequency, and technique are all managed with your specific situation in mind.